INTRODUCTION
Cervical artery dissection (CAD) is an important cause of stroke in younger patients. It accounts for 2.5% of all stroke cases and 5% to 22% of those under 45 years of age [1]. It is classified based on the artery involved (vertebral vs. carotid) and the location of the dissected artery (intracranial vs. extracranial). The most common form is an extracranial internal carotid artery (ICA) dissection [2]. During CAD, arterial blood enters into the vessel wall through the damaged carotid intima and separates the intimal and media layers. This process leads to formation of an intramural hematoma, resulting in stenosis or occlusion. Therefore, CAD can cause thrombosis and vascular stenosis leading to ischemic stroke or transient ischemic attack [3]. Once thought to be rare, with recent progress in vessel luminal imaging, CAD is increasingly recognized as a cause of stroke, particularly in young people. Herein, we report a case of transient ischemic attack with carotid artery dissection caused by Eagle syndrome.
CASE REPORT
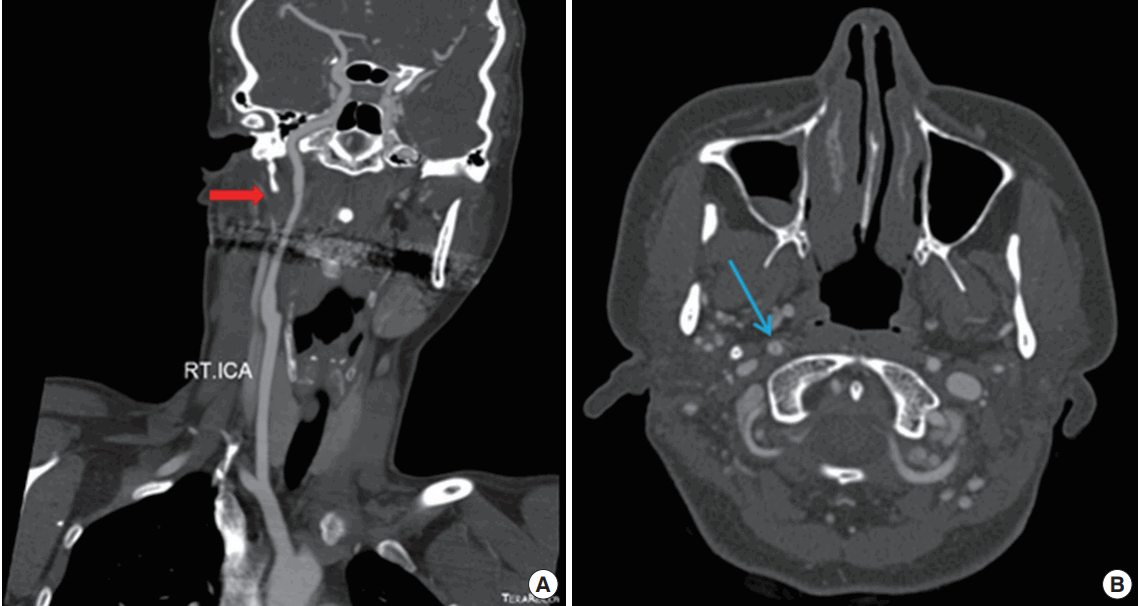
A 38-year-old previously healthy female visited a local hospital with sudden onset of headache and left perioral area numbness that began a few days prior to presentation. There was no associated weakness or other focal neurologic deficit. Non-contrast head computed tomography (CT) was unremarkable. CT angiography (CTA) of the head and neck showed decreased flow in the right ICA (Fig. 1A, B). Magnetic resonance imaging (MRI) showed no acute infarction on diffusion-weighted imaging; however, magnetic resonance angiography (MRA) showed decreased flow in the right ICA. Conventional angiography showed severe luminal narrowing in the right ICA (Fig. 1C). The patient was referred to our hospital for further evaluation and management of right ICA stenosis. On admission, her headache and left perioral numbness had improved. We reviewed the brain images and suspected an arterial dissection. Repeat CTA showed elongation of the right styloid process (45 mm), with the tip of the styloid adjacent to the ICA. The tip had slightly compressed the ICA, and was considered to be the cause of the carotid dissection (Fig. 2). The patient received dual antiplatelet therapy (aspirin and clopidogrel). As repeated compression of the recently occluded vessel could lead to recanalization and subsequent thromboembolism, and progression of the dissection on the right side had the potential to cause further cerebral ischemia, surgical resection of the right styloid processes was scheduled. Otorhinolaryngology was consulted and surgical resection of the styloid process was performed using an external approach. No complications occurred during surgery. Repeat CTA at 6 months showed improved flow in the right cervical ICA (Fig. 3). The patient had no further episodes of transient ischemic attack.
DISCUSSION
Typical clinical features of CAD include unilateral neck pain; headache; ipsilateral Horner’s syndrome, followed by manifestations of cerebral or ocular ischemia; and cranial nerve palsies [2]. CAD can result from traumatic or spontaneous dissection. Most dissections involve minor trauma, stretch, or mechanical stress. Chiropractic manipulation can also cause CAD [4]. The etiology of spontaneous dissection is thought to be multifactorial. Congenital and acquired abnormalities of the connective tissue in the arterial media or elastica and edema of the arterial wall can promote dissection. For example, Marfan syndrome, cystic medial necrosis, fibromuscular dysplasia, and migraine are conditions that are found more often than expected in patients with arterial dissection [5]. Ultrastructural connective tissue abnormalities of collagen and the extracellular matrix have occasionally been found in skin biopsies taken from patients with arterial dissection [6].
Until recently, catheter angiography was the method of choice to diagnose arterial dissection; however, with the advent of Doppler ultrasonography, MRI/MRA, and CTA, most dissections can now be diagnosed noninvasively [2]. The American Heart Association, American Stroke Association, and the International Headache Society all recommend MRI/ MRA with fat suppression as the best initial screening test for dissection [7,8]. CTA is also considered useful, especially if there is doubt about the diagnosis or the dissection is at a very early stage [7,8].
Treatment remains empiric and is guided by clinician discretion on a case-by-case basis. Options for treatment include intravenous and intra-arterial thrombolysis, surgical repair, anticoagulation, and antiplatelet medication [9]. Thrombolysis is currently recommended for patients with CAD who meet criteria and have no contraindications. Antiplatelet and anticoagulant agents show similar efficacy. Endovascular and surgical repair is considered a last resort but should be kept in mind, especially for the treatment of patients with recurrent dissection or lack of resolution [9]. The prognosis depends on the severity of neurological deficits, but is generally good in extracranial dissection. The recurrence rate of CAD is very low and patients with a stroke due to dissection tend to have a good long-term outcome, with 75% being functionally independent at 3 months [10].
Eagle syndrome is caused by an elongated styloid process or a calcified stylohyoid and stylomandibular ligament [11]. The elongated styloid process may compress the glossopharyngeal nerve and surrounding structures, causing recurrent odynophagia and cervical pain. These clinical features were first described by Eagle in 1937; hence, the symptoms associated with an elongated styloid process became known as Eagle syndrome. Stylocarotid artery syndrome is attributed to extracranial impingement of the ICA by a deviated and elongated styloid process. The syndrome may present with dissection of the carotid artery, resulting in a transient ischemic attack or stroke [12]. Only a few case reports have described arterial dissection due to Eagle syndrome. The optimal treatment, including surgical resection of the styloid process, remains unclear, and requires further investigation.
In conclusion, CAD is a major cause of stroke in young adults. The primary goals of treatment are to promptly save at-risk brain tissue and prevent additional ischemia or stroke recurrence. Therefore, the identification of the pathophysiology underlying CAD is required in order to estimate the risk of recurrent cerebral ischemia and to select optimal treatment methodology. Although Eagle syndrome is a rare cause of CAD, it can be treated with surgical resection. Therefore, when the cause of CAD is unclear, it is necessary to determine whether the distal portion of the styloid process is in close contact with the carotid artery.